
A comprehensive guide to stool and microbiome testing
This article was originally published in June 2018 as “The benefits of comprehensive stool testing” and was updated in October 2021 to reflect the latest research, my updated testing philosophy, and current recommended tests.
Stool and microbiome testing can help identify bacterial imbalances, yeast infections, parasites, and more. But not all stool tests are accurate, and some can be flat-out misleading. Read on to learn about the various types of stool and microbiome tests, and which tests are the most useful and reliable.
Interest in the gut microbiome and the role of gut health in shaping our overall health has grown tremendously in recent years. Many companies have emerged to meet the growing demand for a better understanding of our inner microbial worlds.
Anyone can now buy an at-home microbiome test and receive personalized tips as to what probiotics to take or what diet to eat. But are these tests accurate, and is there evidence to support such recommendations?
In this article, I’ll discuss what stool tests are, who might benefit from them, and the different methods used for stool testing. I’ll also review some of the most popular commercially available tests. If you’re just interested in which stool and microbiome tests I currently use and recommend, feel free to jump to the takeaways section at the end.
Prefer audio? Check out my recent podcast with Eileen Laird all about stool testing.
What is a comprehensive stool test?
A comprehensive stool test is any test that provides more detailed information about gut health, beyond a standard stool culture. They typically provide information about:
- Beneficial bacteria and overall bacterial balance
- Gut pathogens, including potentially pathogenic bacteria, yeasts, and parasites
- Overall gut health, including things like digestion, absorption, immune function, inflammation, and short-chain fatty acids
- Potential signs of inflammatory bowel disease, colorectal cancer, or other more serious gut conditions
Most gut microbiome tests are not comprehensive tests. Instead, they provide a closer look at the overall balance of gut bacteria using more thorough DNA sequencing.
Both comprehensive stool tests and gut microbiome tests can be useful and, as we’ll see later, they can often complement one another.
Who should get comprehensive stool or microbiome testing?
You might particularly benefit from more extensive stool and microbiome testing if you have any of the following symptoms or conditions:
- Digestive issues
- Acid reflux (GERD)
- Gas or bloating
- Abdominal pain
- Constipation
- Diarrhea
- Irritable bowel syndrome
- Inflammatory bowel disease
- Diverticulitis
- Rapid weight gain or weight loss
Those with other symptoms outside of the gut might also benefit from comprehensive stool and/or microbiome testing:
- Food intolerances
- Rashes or hives
- Acne
- Mood disturbances
- Depression or anxiety
- Fatigue
- Insomnia
- Brain fog
- Joint pain
- Chronic sinus issues or allergies
Note that the latter group of symptoms can originate from several underlying causes, some of which are not related to the gut. If symptoms persist after addressing diet and lifestyle factors though, it may be a good idea to determine if any major gut pathologies are present.
The different types of stool & microbiome tests
In this section, I discuss the pros and cons of stool testing methods and which companies are currently using them. If you don’t care for the details, feel free to skip to the next section!
There are many different methods currently being used for stool and microbiome testing. Unfortunately, not all of them are accurate or clinically useful. Stool tests can be broadly divided into two major categories: culture-based tests and molecular-based tests.
1) Culture-based stool tests
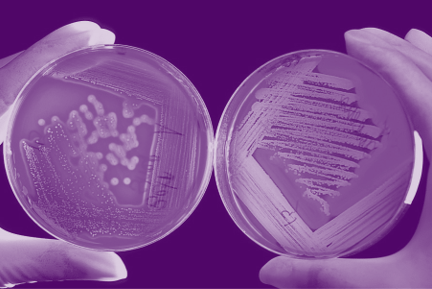
The scientific study of gut microbes relied on culture for decades. This is where scientists add a small amount of a stool sample to a petri dish in the lab and look at it under a microscope following an incubation period. They can also apply different stains to the microbes to look for different characteristics.
The problem is that culture favors rapidly growing, oxygen-loving microbes, whereas most of the microbes in the human gut are anaerobic (oxygen-intolerant) bacteria. This means that most of the important bacteria in the human gut cannot be effectively studied by culture. In fact, we now know that culture-based methods miss about 95 percent of the human gut microbiome!
Moreover, culture-based methodologies cannot tell you the actual abundance of microbes in the original sample. Many microbes can make up only 0.001% of a stool sample but will grow rapidly when exposed to lab culture conditions. This can lead to inappropriate diagnoses of bacterial overgrowth and unnecessary antimicrobial or antibiotic treatments.
Popular companies/tests that use stool culture: Doctor’s Data (Comprehensive Stool Analysis), Genova (Comprehensive Digestive Stool Analysis)
2) DNA-based or molecular techniques
With the arrival of DNA and RNA sequencing, microbiome research quickly moved away from culture towards sequencing-based approaches. For the first time, scientists could assess many microbes in a sample without the need to culture them first. There are several DNA-based approaches that are currently used in both research and commercial laboratory settings:
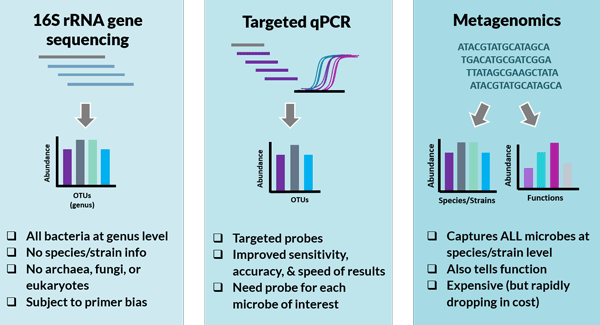
16S rRNA gene sequencing
This method is very cost-effective and is widely used to characterize the bacterial community in research settings. 16S rRNA gene sequencing (16S) is based on sequencing a particular gene that all bacteria have as part of their bacterial ribosome. Like a bacterial fingerprint, this gene can help distinguish one bacterium from another. By matching these “fingerprints” up to a known database of sequences, we can learn which bacteria are present and in what abundance, and with pretty good accuracy down to the genus level. However, 16S is less accurate at the species level, and does not provide any information about fungi or parasites.
Popular companies: Thryve, Biohm, AmericanGut, Atlas BioMed, uBiome (no longer available)
Targeted or quantitative PCR
This method uses specific short sequences called primers to look for specific microbes. Targeted or quantitative PCR (qPCR) is more sensitive than 16S, allowing identification of specific microbes at the genus or species level. However, the utility of targeted or quantitative PCR for assessing the gut ecosystem depends on how many primers a specific lab uses, and which microbes they choose to profile. For example, a lab with primers for 20 of the most abundant commensal microbes and 15 common pathogenic species in the human gut would likely be more useful than a laboratory that only assesses five common pathogens.
Popular companies: Genova (GI Effects), Doctor’s Data (GI 360), Diagnostic Solutions (GI-MAP), Vibrant Wellness
Metagenomics
This method, also called whole genome, next-generation, or shotgun sequencing, uses deep sequencing to identify every single gene in the gut microbiome known to science. Metagenomics is the most accurate method for determining the relative and absolute abundance of microbes and has the highest resolution, often down to the strain level. It can also provide information about the functional capabilities of microbes. It is more expensive than other molecular approaches, though advances in sequencing technology is increasingly making it more affordable.
Popular companies: Thorne (previously Onegevity), Microbiome Labs, DayTwo, Aperiomics, Sun Genomics, SmartDNA (Australia), Microba (Australia)
Meta-transcriptomics and metabolomics
These high-throughput techniques assess the metabolic output of the gut microbiome and the sum total of all of the gene expression of the microbiome, respectively. While metagenomics asks the question “who is there?”, meta-transcriptomics and metabolomics ask the question “what are they doing?”. In the near future, these techniques will likely complement other molecular approaches in a way that is clinically relevant and actionable – but for now, they are impractical for clinical use. Most companies using this and making recommendations are way out ahead of the science.
Popular companies: Viome
Why you should never make clinical treatment decisions based on culture-based stool test results
If you’re still not convinced that culture is inaccurate for assessing bacterial abundance, hopefully this example will help. Here is a stool bacteriology culture report from Doctor’s Data:
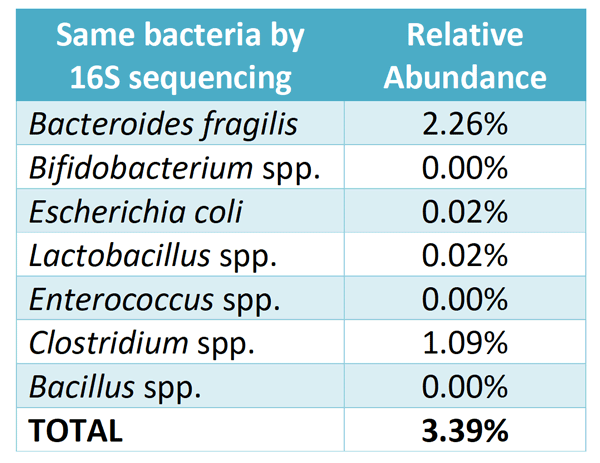
Here is the exact same stool sample run through 16S rRNA sequencing. I downloaded the raw data from uBiome and extracted only the microbes that were reported on Doctor’s Data:
You can see that the bacteria picked up by culture-based methods represents only 3.39% of the total bacteria present in the stool sample. It also completely skews the relative abundance, with both Bacteroides fragilis (2.26%) and Enterococcus (0.00%) reported as a 4+.
This is something that I can’t emphasize enough: NEVER make clinical decisions based on culture-based testing alone! If you see a 4+ for a pathogen like Pseudomonas aeruginosa or Citrobacter freundii, do NOT treat until you have followed up with a sensitive PCR-based test. Nine and a half times out of ten, the microbe in question will represent less than 0.001% of the actual gut ecosystem. I have seen so many people harmed by treating for a microbe picked up on culture that was likely never a problem in the first place.
Other common mistakes with stool testing
Mistake #1: Assuming that the test-generated diet and supplement recommendations are personalized and 100% applicable to your case. Many gut test reports will provide recommendations about which probiotics to take, which prebiotic fiber, or certain gut supplements. While these recommendations often appear personalized, in most cases they are selecting between one of a few generic options to present to you. Most of the recommendations are not based on evidence and are simply a push to buy a certain product.
Mistake #2: Becoming overly concerned with your abundance of one or two microbes, rather than focusing on the overall picture. Everyone loves data, myself included. But it’s important to remember that the gut is a complex system, that there is a lot of variation in what is considered a healthy microbiome, and also variation from day-to-day! I always encourage people to refrain from fretting over increasing or decreasing microbe X or microbe Z. At this point, we should primarily be using stool testing as a way to look for major red flags. Beyond that, we can also use overall patterns to generate hypotheses about what therapeutic approaches might be worth trying. At the end of the day though, how an intervention affects your overall symptoms and quality of life is much more important than whether you have the optimal abundance of Akkermansia!
An analysis of popular stool & microbiome tests
Alright, I’m sure this is the part you’ve all been waiting for! Just a reminder that I have no affiliation with any of these companies. This is simply my best attempt at an objective, independent analysis of the available testing options.
Thryve
Cost: $99, available directly from their website
Methodology: 16S rRNA sequencing
Clinical markers: no
Tests for parasites/yeast: no
Other comments: Profiles all bacteria down to the genus level and offers customized probiotics and food recommendations. Many people who were using previously using uBiome for serial microbiome testing have since switched to Thryve. It’s important to note, however, that the results of the two are not directly comparable since Thryve uses slightly different primers for their sequencing.
Verdict: inexpensive but limited to bacteria at higher taxonomic levels. Choose this test if you are just interested to explore your gut bacteria and don’t need clinically actionable information.
BIOHM Gut Test
Cost: $129, available directly from their website
Methodology: 16S rRNA sequencing + ITS (the equivalent of 16S for gut fungi/yeast)
Clinical markers: no
Tests for parasites/yeast: yes for yeast, no for parasites
Other comments: Profiles all bacteria and fungi down to the genus level. Not sure I trust the relative abundances on some of the reports I’ve seen – this may be due to the particular primers the lab uses.
Verdict: relatively inexpensive and a bit broader in scope since it includes fungi. An okay choice for just exploring the bacteria and fungi in your microbiome, but not the best choice for clinically actionable information.
Viome Health Intelligence Test
Cost: $179, available directly from their website
Methodology: meta-transcriptomics
Clinical markers: no
Tests for parasites/yeast: no, though may detect some via RNA
Other comments: Meta-transcriptomics is a legitimate methodology based on sequencing the RNA of microbes. Unfortunately, the idea that we know what to do with this information or can make clinical or dietary recommendations based on it is far ahead of any solid science.
Verdict: this test has largely become popular because of good marketing and plays on the fact that most people don’t understand that this is way out ahead of the science. I don’t recommend this test.
Diagnostic Solutions GI-MAP
Cost: $200-400, depending on your practitioner and insurance
Methodology: quantitative PCR
Clinical markers: yes, but questionable accuracy (see below)
Tests for parasites/yeast: yes
Other comments: Identical split samples sent to the lab revealed some issues with test accuracy, with wide variability in some of the clinical markers like calprotectin. The response from the CEO was disappointing and made no indication that they cared or would make any effort to resolve the issue. Markers unique to this test include H pylori virulence factors and anti-gliadin IgA.
Verdict: I still review GI-MAP test results but am no longer confident enough in the reliability of the results or integrity of the company to recommend them.
Vibrant Wellness Gut Zoomer
Cost: $200-400, depending on your practitioner
Methodology: Microarray (similar to qPCR but higher throughput)
Clinical markers: yes
Tests for parasites/yeast: yes
Other comments: Several unique clinical markers, including beta defensin 2, S100A12, MMP9, and bile acid metabolites. However, some of the abundances and reference ranges for bacteria seem somewhat arbitrary and do not offer any way to look at the relative balance of bacteria.
Verdict: Not a preferred test, though I have seen less of these overall and haven’t had the chance to evaluate it as thoroughly as some other tests.
Doctor’s Data or Genova Comprehensive Stool Analysis w/ Parasitology (GOOD CHOICE for clinical markers)
Cost: $300-350
Methodology: Culture / microscopy
Clinical markers: no
Tests for parasites/yeast: yes
Other comments: Was one of the most popular tests on the market, and many practitioners still order this test. We now know that the culture-based section of this test is completely inaccurate. However, it is still useful for the parasitology and clinical markers, if combined with a PCR-based test to look for bacteria.
Verdict: A solid choice for clinical markers and traditional parasitology screening. Important to completely ignore the culture-based section.
Doctor’s Data GI 360
Cost: $300-500, depending on whether you order through a practitioner or via direct-to-consumer laboratories
Methodology: PCR, microscopy, and culture
Clinical markers: yes
Tests for parasites/yeast: yes
Other comments: Clinical markers unique to this test include stool mucus, carbohydrate digestion/absorption, lactoferrin, and lysozyme.
Verdict: A great comprehensive overview of gut health complete with clinical markers. This test is very similar to the Genova GI Effects (see below). Unfortunately, they still include a page of culture-based results, which are not an accurate way to assess gut bacteria and should be ignored.
Genova GI Effects Comprehensive Profile – TOP CHOICE
Cost: $300-500, depending on whether you order through a practitioner or via direct-to-consumer laboratories
Primary methodology: PCR, microscopy, and culture
Clinical markers: yes
Tests for parasites/yeast: yes
Other notes: Clinical makers unique to this test include eosinophil protein X. Lactoferrin, H pylori antigen, and KOH preparation for yeast are available as add-on tests.
The GI Effects is also unique among the comprehensive stool tests in that it includes Methanobrevibacter (the dominant methanogen in the human gut) and Desulfovibrio (one of the most common hydrogen sulfide producers).
The lab also recently added Blastocystis reflex subtyping, meaning that if Blastocystis is detected via PCR, it will automatically determine which subtype is present. This may have more clinical utility as we learn more about Blastocystis subtypes.
Verdict: A great comprehensive overview of gut health complete with clinical markers. This test is very similar to the Doctor’s Data GI 360, but I have a slight preference for the GI Effects because of the inclusion of methanogens and sulfate-reducing bacteria, and their easier-to-read report. Unfortunately, they also include a page of culture-based results, which are not an accurate way to assess gut bacteria and should be ignored. This is currently my go-to all-in-one comprehensive stool test.
Sun Genomics
Cost: $169, available directly from their website
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, but they don’t seem to include these in the report
Details: No raw data available. Surprising that they don’t include yeast, archaea, or viruses in their report, since this is one of the main advantages of metagenomics, other than being able to et down to species/strain level! They could also do a lot more in terms of reporting bacterial functional capacity.
Verdict: a decent option, but not worth the price given that the real benefit of metagenomics is the depth of sequencing and getting the raw data, which they do not provide.
Aperiomics Xplore-Microbiome
Cost: $$$, requires practitioner to order
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes
Details: The report includes all identified microbes ≥ 0.1% relative abundance, at the species level. Because they specialize in using metagenomics for pathogen detection, they do not offer a way to see the breakdown at higher taxonomic levels, and there is no raw data provided.
Verdict: reports are specialized for pathogen detection only. Not the best choice for looking at overall gut balance, as there is no way to see the data at various taxonomic levels.
Microbiome Labs BiomeFX
Cost: $300-400, depending on the practitioner you order through
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, small number included in report
Other notes: they offer a detailed consumer-friendly report, including information about microbial functions, vitamin production, and short-chain fatty acid production capacity. Unfortunately, it does not appear that they provide access to the raw data. This is a newer test and one I will continue to evaluate as I see more of them.
Verdict: A solid option for metagenomics and their report is quite consumer-friendly. However, no access to the raw data, requires a practitioner to order, and is currently a bit more expensive than other comparable metagenomic tests.
Thorne Gut Health Test (Onegevity) – TOP CHOICE
Cost: $198, available directly from their website
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, available in raw data
Other notes: This metagenomics test was initially launched as Onegevity GutBio and acquired by Thorne in 2021. They offer a detailed consumer report, including microbial functions, vitamin biosynthesis, and short-chain fatty acid-producing capacity. The raw data, available as a downloadable Excel file, is excellent for looking at bacterial balance and screening for stealth infections that may not be picked up with other PCR methods. Results currently take about 6-8 weeks from sample submission.
Verdict: I’m a big fan of this test and it is my current go-to test for assessing the overall microbiome. The consumer summary reports have improved significantly and the raw data is research-level quality. This test is particularly good for assessing bacterial abundance, overall microbial function, and screening for stealth gut infections. Note that it does not provide clinical markers, and the diet and supplement recommendations provided in the report are often contradictory and not necessarily evidence-based.
FAQ
Does everyone need a gut test?
No. If you’re healthy, there is no reason you need stool testing, unless you’re just interested to learn more about the microbiome! Even if you’re struggling with chronic health issues, your first step should be getting the major health behaviors in place, as this can often significantly improve symptoms. If you’re still struggling with symptoms once you’ve optimized your diet and lifestyle, it could be worth testing your gut to determine if it’s contributing to your health problems.
What if my GI doc already ran a stool test?
Your doctor’s office is likely only testing that sample for about 0.01% of what they could be testing your gut for. Here’s a typical result from a basic lab stool culture:
No visible ova or parasites
Occult blood: negative
Appearance: normal
Not only does this result provide little useful information, but it can also lead you to believe your gut is healthy, even if gut pathologies are the underlying cause of your health struggles.
Depending on your symptoms, a GI doc may also run a basic PCR screen for some of the most common parasites, but these are far from comprehensive.
How often should I get a stool test?
For most people, a single test is enough as a screening tool. If the test identifies a parasite or something that clearly needs to be treated, then it is often a good idea to get a follow-up test to confirm that it was cleared.
Some people like to get more frequent tests to be able to track things over time, and this can certainly be interesting and occasionally help generate hypotheses to guide treatment, but it’s important not to get too fussy over the numbers, and instead focus on whether your symptoms and quality of life are improving.
Is qPCR effective for detecting parasites?
Yes. Several recent studies and literature reviews suggest that qPCR detection of parasites is equivalent, and in many cases superior, to microscopy-based parasitology.4–9 Not only can qPCR detect the absence or presence of parasites, but it can also detect parasite load by providing an absolute number per gram of stool. Unlike traditional microscopy, this method does not require stool sampling on multiple days to ensure that parasites are detected and offers more rapid results. That being said, some parasites are still picked up more frequently by traditional parasitology, so combining the two methods is the most thorough way to screen for parasites.
What about the MALDI-TOF with high complexity culture method, isn’t that better than basic stool culture?
In recent years, there has been a resurgence of interest in culture-based methodologies thanks to improvements in culture techniques and a newer detection method called MALDI-TOF. MALDI-TOF uses mass spectrometry of microbial proteins and can identify over 1,400 microbial species without having to purify or isolate them.
The MALDI-TOF method has been shown to have 99 percent accuracy in the ID of common commensal microbes, 100 percent accuracy in ID of common pathogenic species, and high reproducibility across laboratories.1,2 The problem is that MALDI-TOF still relies on successfully culturing the microbe first. And even with high-complexity stool cultures now used in some commercial laboratories, they still miss 95 percent of the microbiome!
Are fecal SCFAs reliable?
Somewhat. Short-chain fatty acids (SCFAs) are produced from the bacterial fermentation of dietary fiber and play important roles in the health of the gut and the rest of the body. However, quantifying them poses quite a challenge. Fecal excretion of SCFAs depends on the rate of absorption, cross-feeding interactions, and gut motility, so fecal SCFAs do not directly reflect SCFA production in the gut. For instance, ulcerative colitis patients have impaired absorption of butyrate, which means they will excrete a greater proportion of the butyrate they produce. One recent study also found that higher fecal SCFA excretion, which is typically thought to be indicative of good gut health, was associated with obesity, hypertension, and cardiometabolic disease risk factors.10 In general though, low fecal SCFAs do tend to correlate with lower SCFA production.
Is zonulin a useful marker of gut permeability?
No. Blood or fecal zonulin has been shown to be elevated in depression, autism, diabetes, metabolic syndrome, PCOS, aging, and celiac disease. However, only a fraction of the patients in these studies have elevated zonulin.11,12 Moreover, many of the studies used to support the clinical use of zonulin testing were not measuring zonulin at all – they were measuring properdin, a zonulin analog.13
Furthermore, zonulin is only weakly correlated with other more validated measures of intestinal permeability, such as the differential sugar (lactulose-mannitol) absorption test and has been shown to fluctuate greatly throughout the day.11,12 Zonulin antibodies in the blood may be more stable and reflective of intestinal permeability, but these obviously will not be included on a stool test.
Does the stool microbiome actually reflect the gut microbiome?
You might recall a study that I reviewed and discussed on Chris Kresser’s podcast, which suggests that stool samples don’t accurately reflect the gut microbiome, and tend to over or underrepresent different genera from even the most distal part of the colon.
But this doesn’t mean that stool testing is useless. Consider that the majority of published research on the human gut microbiome to date is on fecal samples. In fact, given the current lack of human studies on the gut mucosa, a stool sample is likely more clinically useful than a small intestinal microbial biopsy.
If you think about it:
- We know how certain interventions like diet, exercise, and antibiotics affect the fecal microbiome.
- We know which fecal microbiome patterns are correlated with certain diseases
- We have a general idea of which microbes should make up the bulk of a healthy fecal sample
- We have a general idea of which microbes should not be present in large amounts in fecal samples.
This means that while fecal samples are imperfect, they are still a useful proxy for the overall ecosystem and are currently one of the best ways to screen for various gut pathologies.
Summary: tests I currently recommend and use myself and with clients
In summary, comprehensive stool tests and microbiome tests can be very helpful tools, but it’s essential to know which ones are reliable, and how to use the information appropriately. The testing landscape is constantly changing, so I am always re-evaluating different stool testing options and will attempt to keep this article up to date with what is available!
I have no affiliation with any stool testing companies. As of this writing, I recommend:
1) Genova GI Effects Comprehensive Profile
This test provides the most comprehensive look at the overall gut environment, parasites, and gives a decent look at bacterial balance. If you’re new to exploring gut health and are only going to get one test, I’d go with this one.
GI Effects is available through many functional medicine practitioners, or direct-to-consumer via directlabs.com (Click on “Order Tests” and search for “GI Effects”).
I recommend the 3-day stool collection if this is your first comprehensive stool test, as it is slightly more thorough in looking for parasites. Results typically take 2 weeks.
2) Thorne Gut Health Test + Genova GI Effects Comprehensive (or CSAP)
For a deeper dive into gut health, I recommend combining the Thorne Gut Health Test with the GI Effects, or another test that will provide clinical information about the gut environment, like the CSAP (just be sure to ignore the culture section!).
Thorne provides the best and most thorough look at the gut microbiome, with extensive raw data that includes overall bacterial balance and the ability to screen for stealth infections. The Thorne Gut Health test is available directly from their website for $198. Results typically take 4-8 weeks.
Unfortunately, the consumer report from Thorne is pretty limited. If you’d like help exploring and understanding your raw data, this is something that I do as part of my 1-on-1 health consultations.
Have you had comprehensive stool testing? Please share your thoughts or experience in the comments below!

About Lucy
Lucy Mailing, PhD is an independent microbiome researcher and gut health science educator. She writes evidence-based articles about the microbiome, gut health, and nutrition science, inspired by her own health journey overcoming chronic eczema.

A comprehensive guide to stool and microbiome testing
This article was originally published in June 2018 as “The benefits of comprehensive stool testing” and was updated in October 2021 to reflect the latest research, my updated testing philosophy, and current recommended tests.
Stool and microbiome testing can help identify bacterial imbalances, yeast infections, parasites, and more. But not all stool tests are accurate, and some can be flat-out misleading. Read on to learn about the various types of stool and microbiome tests, and which tests are the most useful and reliable.
Interest in the gut microbiome and the role of gut health in shaping our overall health has grown tremendously in recent years. Many companies have emerged to meet the growing demand for a better understanding of our inner microbial worlds.
Anyone can now buy an at-home microbiome test and receive personalized tips as to what probiotics to take or what diet to eat. But are these tests accurate, and is there evidence to support such recommendations?
In this article, I’ll discuss what stool tests are, who might benefit from them, and the different methods used for stool testing. I’ll also review some of the most popular commercially available tests. If you’re just interested in which stool and microbiome tests I currently use and recommend, feel free to jump to the takeaways section at the end.
Prefer audio? Check out my recent podcast with Eileen Laird all about stool testing.
What is a comprehensive stool test?
A comprehensive stool test is any test that provides more detailed information about gut health, beyond a standard stool culture. They typically provide information about:
- Beneficial bacteria and overall bacterial balance
- Gut pathogens, including potentially pathogenic bacteria, yeasts, and parasites
- Overall gut health, including things like digestion, absorption, immune function, inflammation,
- and short-chain fatty acids
- Potential signs of inflammatory bowel disease, colorectal cancer, or other more serious gut conditions
Most gut microbiome tests are not comprehensive tests. Instead, they provide a closer look at the overall balance of gut bacteria using more thorough DNA sequencing.
Both comprehensive stool tests and gut microbiome tests can be useful and, as we’ll see later, they can often complement one another.
Who should get comprehensive stool or microbiome testing?
You might particularly benefit from more extensive stool and microbiome testing if you have any of the following symptoms or conditions:
- Digestive issues
- Acid reflux (GERD)
- Gas or bloating
- Abdominal pain
- Constipation
- Diarrhea
- Irritable bowel syndrome
- Inflammatory bowel disease
- Diverticulitis
- Rapid weight gain or weight loss
Those with other symptoms outside of the gut might also benefit from comprehensive stool and/or microbiome testing:
- Food intolerances
- Rashes or hives
- Acne
- Mood disturbances
- Depression or anxiety
- Fatigue
- Insomnia
- Brain fog
- Joint pain
- Chronic sinus issues or allergies
Note that the latter group of symptoms can originate from several underlying causes, some of which are not related to the gut. If symptoms persist after addressing diet and lifestyle factors though, it may be a good idea to determine if any major gut pathologies are present.
The different types of stool & microbiome tests
In this section, I discuss the pros and cons of stool testing methods and which companies are currently using them. If you don’t care for the details, feel free to skip to the next section!
There are many different methods currently being used for stool and microbiome testing. Unfortunately, not all of them are accurate or clinically useful. Stool tests can be broadly divided into two major categories: culture-based tests and molecular-based tests.
1) Culture-based stool tests
The scientific study of gut microbes relied on culture for decades. This is where scientists add a small amount of a stool sample to a petri dish in the lab and look at it under a microscope following an incubation period. They can also apply different stains to the microbes to look for different characteristics.
The problem is that culture favors rapidly growing, oxygen-loving microbes, whereas most of the microbes in the human gut are anaerobic (oxygen-intolerant) bacteria. This means that most of the important bacteria in the human gut cannot be effectively studied by culture. In fact, we now know that culture-based methods miss about 95 percent of the human gut microbiome!
Moreover, culture-based methodologies cannot tell you the actual abundance of microbes in the original sample. Many microbes can make up only 0.001% of a stool sample but will grow rapidly when exposed to lab culture conditions. This can lead to inappropriate diagnoses of bacterial overgrowth and unnecessary antimicrobial or antibiotic treatments.
Popular companies/tests that use stool culture: Doctor’s Data (Comprehensive Stool Analysis), Genova (Comprehensive Digestive Stool Analysis)
2) DNA-based or molecular techniques
With the arrival of DNA and RNA sequencing, microbiome research quickly moved away from culture towards sequencing-based approaches. For the first time, scientists could assess many microbes in a sample without the need to culture them first. There are several DNA-based approaches that are currently used in both research and commercial laboratory settings:
16S rRNA gene sequencing
This method is very cost-effective and is widely used to characterize the bacterial community in research settings. 16S rRNA gene sequencing (16S) is based on sequencing a particular gene that all bacteria have as part of their bacterial ribosome. Like a bacterial fingerprint, this gene can help distinguish one bacterium from another. By matching these “fingerprints” up to a known database of sequences, we can learn which bacteria are present and in what abundance, and with pretty good accuracy down to the genus level. However, 16S is less accurate at the species level, and does not provide any information about fungi or parasites.
Popular companies: Thryve, Biohm, AmericanGut, Atlas BioMed, uBiome (no longer available)
Targeted or quantitative PCR
This method uses specific short sequences called primers to look for specific microbes. Targeted or quantitative PCR (qPCR) is more sensitive than 16S, allowing for the identification of specific microbes at the genus or species level. However, the utility of targeted or quantitative PCR for assessing the gut ecosystem depends on how many primers a specific lab uses, and which microbes they choose to profile. For example, a lab with primers for 20 of the most abundant commensal microbes and 15 common pathogenic species in the human gut would likely be more useful than a laboratory that only assesses five common pathogens.
Popular companies: Genova (GI Effects), Doctor’s Data (GI 360), Diagnostic Solutions (GI-MAP), Vibrant Wellness
Metagenomics
This method, also called whole genome, next-generation, or shotgun sequencing, uses deep sequencing to identify every single gene in the gut microbiome known to science. Metagenomics is the most accurate method for determining the relative and absolute abundance of microbes and has the highest resolution, often down to the strain level. It can also provide information about the functional capabilities of microbes. It is more expensive than other molecular approaches, though advances in sequencing technology is increasingly making it more affordable.
Popular companies: Thorne (previously Onegevity), Microbiome Labs, DayTwo, Aperiomics, Sun Genomics, SmartDNA (Australia), Microba (Australia)
Meta-transcriptomics and metabolomics
These high-throughput techniques assess the metabolic output of the gut microbiome and the sum total of all of the gene expression of the microbiome, respectively. While metagenomics asks the question “who is there?”, meta-transcriptomics and metabolomics ask the question “what are they doing?”. In the near future, these techniques will likely complement other molecular approaches in a way that is clinically relevant and actionable – but for now, they are impractical for clinical use. Most companies using this and making recommendations are way out ahead of the science.
Popular companies: Viome
Why you should never make clinical treatment decisions based on culture-based stool test results
If you’re still not convinced that culture is inaccurate for assessing bacterial abundance, hopefully this example will help. Here is a stool bacteriology culture report from Doctor’s Data:
Here is the exact same stool sample run through 16S rRNA sequencing. I downloaded the raw data from uBiome and extracted only the microbes that were reported on Doctor’s Data:
You can see that the bacteria picked up by culture-based methods represents only 3.39% of the total bacteria present in the stool sample. It also completely skews the relative abundance, with both Bacteroides fragilis (2.26%) and Enterococcus (0.00%) reported as a 4+.
This is something that I can’t emphasize enough: NEVER make clinical decisions based on culture-based testing alone! If you see a 4+ for a pathogen like Pseudomonas aeruginosa or Citrobacter freundii, do NOT treat until you have followed up with a sensitive PCR-based test. Nine and a half times out of ten, the microbe in question will represent less than 0.001% of the actual gut ecosystem. I have seen so many people harmed by treating for a microbe picked up on culture that was likely never a problem in the first place.
Other common mistakes with stool testing
Mistake #1: Assuming that the test-generated diet and supplement recommendations are personalized and 100% applicable to your case. Many gut test reports will provide recommendations about which probiotics to take, which prebiotic fiber, or certain gut supplements. While these recommendations often appear personalized, in most cases they are selecting between one of a few generic options to present to you. Most of the recommendations are not based on evidence and are simply a push to buy a certain product.
Mistake #2: Becoming overly concerned with your abundance of one or two microbes, rather than focusing on the overall picture. Everyone loves data, myself included. But it’s important to remember that the gut is a complex system, that there is a lot of variation in what is considered a healthy microbiome, and also variation from day-to-day! I always encourage people to refrain from fretting over increasing or decreasing microbe X or microbe Z. At this point, we should primarily be using stool testing as a way to look for major red flags. Beyond that, we can also use overall patterns to generate hypotheses about what therapeutic approaches might be worth trying. At the end of the day though, how an intervention affects your overall symptoms and quality of life is much more important than whether you have the optimal abundance of Akkermansia!
An analysis of popular stool & microbiome tests
Alright, I’m sure this is the part you’ve all been waiting for! Just a reminder that I have no affiliation with any of these companies. This is simply my best attempt at an objective, independent analysis of the available testing options.
Thryve
Cost: $99, available directly from their website
Methodology: 16S rRNA sequencing
Clinical markers: no
Tests for parasites/yeast: no
Other comments: Profiles all bacteria down to the genus level and offers customized probiotics and food recommendations. Many people who were using previously using uBiome for serial microbiome testing have since switched to Thryve. It’s important to note, however, that the results of the two are not directly comparable since Thryve uses slightly different primers for their sequencing.
Verdict: inexpensive but limited to bacteria at higher taxonomic levels. Choose this test if you are just interested to explore your gut bacteria and don’t need clinically actionable information.
BIOHM Gut Test
Cost: $129, available directly from their website
Methodology: 16S rRNA sequencing + ITS (the equivalent of 16S for gut fungi/yeast)
Clinical markers: no
Tests for parasites/yeast: yes for yeast, no for parasites
Other comments: Profiles all bacteria and fungi down to the genus level. Not sure I trust the relative abundances on some of the reports I’ve seen – this may be due to the particular primers the lab uses.
Verdict: relatively inexpensive and a bit broader in scope since it includes fungi. An okay choice for just exploring the bacteria and fungi in your microbiome, but not the best choice for clinically actionable information.
Viome Health Intelligence Test
Cost: $179, available directly from their website
Methodology: meta-transcriptomics
Clinical markers: no
Tests for parasites/yeast: no, though may detect some via RNA
Other comments: Meta-transcriptomics is a legitimate methodology based on sequencing the RNA of microbes. Unfortunately, the idea that we know what to do with this information or can make clinical or dietary recommendations based on it is far ahead of any solid science.
Verdict: this test has largely become popular because of good marketing and plays on the fact that most people don’t understand that this is way out ahead of the science. I don’t recommend this test.
Diagnostic Solutions GI-MAP
Cost: $200-400, depending on your practitioner and insurance
Methodology: quantitative PCR
Clinical markers: yes, but questionable accuracy (see below)
Tests for parasites/yeast: yes
Other comments: Identical split samples sent to the lab revealed some issues with test accuracy, with wide variability in some of the clinical markers like calprotectin. The response from the CEO was disappointing and made no indication that they cared or would make any effort to resolve the issue. Markers unique to this test include H pylori virulence factors and anti-gliadin IgA.
Verdict: I still review GI-MAP test results but am no longer confident enough in the reliability of the results or integrity of the company to recommend them.
Vibrant Wellness Gut Zoomer
Cost: $200-400, depending on your practitioner
Methodology: Microarray (similar to qPCR but higher throughput)
Clinical markers: yes
Tests for parasites/yeast: yes
Other comments: Several unique clinical markers, including beta defensin 2, S100A12, MMP9, and bile acid metabolites. However, some of the abundances and reference ranges for bacteria seem somewhat arbitrary and do not offer any way to look at the relative balance of bacteria.
Verdict: Not a preferred test, though I have seen less of these overall and haven’t had the chance to evaluate it as thoroughly as some other tests.
Doctor’s Data or Genova Comprehensive Stool Analysis w/ Parasitology (GOOD CHOICE for clinical markers)
Cost: $300-350
Methodology: Culture / microscopy
Clinical markers: no
Tests for parasites/yeast: yes
Other comments: Was one of the most popular tests on the market, and many practitioners still order this test. We now know that the culture-based section of this test is completely inaccurate. However, it is still useful for the parasitology and clinical markers, if combined with a PCR-based test to look for bacteria.
Verdict: A solid choice for clinical markers and traditional parasitology screening. Important to completely ignore the culture-based section.
Doctor’s Data GI 360
Cost: $300-500, depending on whether you order through a practitioner or via direct-to-consumer laboratories
Methodology: PCR, microscopy, and culture
Clinical markers: yes
Tests for parasites/yeast: yes
Other comments: Clinical markers unique to this test include stool mucus, carbohydrate digestion/absorption, lactoferrin, and lysozyme.
Verdict: A great comprehensive overview of gut health complete with clinical markers. This test is very similar to the Genova GI Effects (see below). Unfortunately, they still include a page of culture-based results, which are not an accurate way to assess gut bacteria and should be ignored.
Genova GI Effects Comprehensive Profile – TOP CHOICE
Cost: $300-500, depending on whether you order through a practitioner or via direct-to-consumer laboratories
Primary methodology: PCR, microscopy, and culture
Clinical markers: yes
Tests for parasites/yeast: yes
Other notes: Clinical makers unique to this test include eosinophil protein X. Lactoferrin, H pylori antigen, and KOH preparation for yeast are available as add-on tests.
The GI Effects is also unique among the comprehensive stool tests in that it includes Methanobrevibacter (the dominant methanogen in the human gut) and Desulfovibrio (one of the most common hydrogen sulfide producers).
The lab also recently added Blastocystis reflex subtyping, meaning that if Blastocystis is detected via PCR, it will automatically determine which subtype is present. This may have more clinical utility as we learn more about Blastocystis subtypes.
Verdict: A great comprehensive overview of gut health complete with clinical markers. This test is very similar to the Doctor’s Data GI 360, but I have a slight preference for the GI Effects because of the inclusion of methanogens and sulfate-reducing bacteria, and their easier-to-read report. Unfortunately, they also include a page of culture-based results, which are not an accurate way to assess gut bacteria and should be ignored. This is currently my go-to all-in-one comprehensive stool test.
Sun Genomics
Cost: $169, available directly from their website
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, but they don’t seem to include these in the report
Details: No raw data available. Surprising that they don’t include yeast, archaea, or viruses in their report, since this is one of the main advantages of metagenomics, other than being able to et down to species/strain level! They could also do a lot more in terms of reporting bacterial functional capacity.
Verdict: a decent option, but not worth the price given that the real benefit of metagenomics is the depth of sequencing and getting the raw data, which they do not provide.
Aperiomics Xplore-Microbiome
Cost: $$$, requires practitioner to order
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes
Details: The report includes all identified microbes ≥ 0.1% relative abundance, at the species level. Because they specialize in using metagenomics for pathogen detection, they do not offer a way to see the breakdown at higher taxonomic levels, and there is no raw data provided.
Verdict: reports are specialized for pathogen detection only. Not the best choice for looking at overall gut balance, as there is no way to see the data at various taxonomic levels.
Microbiome Labs BiomeFX
Cost: $300-400, depending on the practitioner you order through
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, small number included in report
Other notes: they offer a detailed consumer-friendly report, including information about microbial functions, vitamin production, and short-chain fatty acid production capacity. Unfortunately, it does not appear that they provide access to the raw data. This is a newer test and one I will continue to evaluate as I see more of them.
Verdict: A solid option for metagenomics and their report is quite consumer-friendly. However, no access to the raw data, requires a practitioner to order, and is currently a bit more expensive than other comparable metagenomic tests.
Thorne Gut Health Test (Onegevity) – TOP CHOICE
Cost: $198, available directly from their website
Methodology: metagenomics
Clinical markers: no
Tests for parasites/yeast: yes, available in raw data
Other notes: This metagenomics test was initially launched as Onegevity GutBio and acquired by Thorne in 2021. They offer a detailed consumer report, including microbial functions, vitamin biosynthesis, and short-chain fatty acid-producing capacity. The raw data, available as a downloadable Excel file, is excellent for looking at bacterial balance and screening for stealth infections that may not be picked up with other PCR methods. Results currently take about 6-8 weeks from sample submission.
Verdict: I’m a big fan of this test and it is my current go-to test for assessing the overall microbiome. The consumer summary reports have improved significantly and the raw data is research-level quality. This test is particularly good for assessing bacterial abundance, overall microbial function, and screening for stealth gut infections. Note that it does not provide clinical markers, and the diet and supplement recommendations provided in the report are often contradictory and not necessarily evidence-based.
FAQ
Does everyone need a gut test?
No. If you’re healthy, there is no reason you need stool testing, unless you’re just interested to learn more about the microbiome! Even if you’re struggling with chronic health issues, your first step should be getting the major health behaviors in place, as this can often significantly improve symptoms. If you’re still struggling with symptoms once you’ve optimized your diet and lifestyle, it could be worth testing your gut to determine if it’s contributing to your health problems.
What if my GI doc already ran a stool test?
Your doctor’s office is likely only testing that sample for about 0.01% of what they could be testing your gut for. Here’s a typical result from a basic lab stool culture:
No visible ova or parasites
Occult blood: negative
Appearance: normal
Not only does this result provide little useful information, but it can also lead you to believe your gut is healthy, even if gut pathologies are the underlying cause of your health struggles.
Depending on your symptoms, a GI doc may also run a basic PCR screen for some of the most common parasites, but these are far from comprehensive.
How often should I get a stool test?
For most people, a single test is enough as a screening tool. If the test identifies a parasite or something that clearly needs to be treated, then it is often a good idea to get a follow-up test to confirm that it was cleared.
Some people like to get more frequent tests to be able to track things over time, and this can certainly be interesting and occasionally help generate hypotheses to guide treatment, but it’s important not to get too fussy over the numbers, and instead focus on whether your symptoms and quality of life are improving.
Is qPCR effective for detecting parasites?
Yes. Several recent studies and literature reviews suggest that qPCR detection of parasites is equivalent, and in many cases superior, to microscopy-based parasitology.4–9 Not only can qPCR detect the absence or presence of parasites, but it can also detect parasite load by providing an absolute number per gram of stool. Unlike traditional microscopy, this method does not require stool sampling on multiple days to ensure that parasites are detected and offers more rapid results. That being said, some parasites are still picked up more frequently by traditional parasitology, so combining the two methods is the most thorough way to screen for parasites.
What about the MALDI-TOF with high complexity culture method, isn’t that better than basic stool culture?
In recent years, there has been a resurgence of interest in culture-based methodologies thanks to improvements in culture techniques and a newer detection method called MALDI-TOF. MALDI-TOF uses mass spectrometry of microbial proteins and can identify over 1,400 microbial species without having to purify or isolate them.
The MALDI-TOF method has been shown to have 99 percent accuracy in the ID of common commensal microbes, 100 percent accuracy in ID of common pathogenic species, and high reproducibility across laboratories.1,2 The problem is that MALDI-TOF still relies on successfully culturing the microbe first. And even with high-complexity stool cultures now used in some commercial laboratories, they still miss 95 percent of the microbiome!
Are fecal SCFAs reliable?
Somewhat. Short-chain fatty acids (SCFAs) are produced from the bacterial fermentation of dietary fiber and play important roles in the health of the gut and the rest of the body. However, quantifying them poses quite a challenge. Fecal excretion of SCFAs depends on the rate of absorption, cross-feeding interactions, and gut motility, so fecal SCFAs do not directly reflect SCFA production in the gut. For instance, ulcerative colitis patients have impaired absorption of butyrate, which means they will excrete a greater proportion of the butyrate they produce. One recent study also found that higher fecal SCFA excretion, which is typically thought to be indicative of good gut health, was associated with obesity, hypertension, and cardiometabolic disease risk factors.10 In general though, low fecal SCFAs do tend to correlate with lower SCFA production.
Is zonulin a useful marker of gut permeability?
No. Blood or fecal zonulin has been shown to be elevated in depression, autism, diabetes, metabolic syndrome, PCOS, aging, and celiac disease. However, only a fraction of the patients in these studies have elevated zonulin.11,12 Moreover, many of the studies used to support the clinical use of zonulin testing were not measuring zonulin at all – they were measuring properdin, a zonulin analog.13
Furthermore, zonulin is only weakly correlated with other more validated measures of intestinal permeability, such as the differential sugar (lactulose-mannitol) absorption test and has been shown to fluctuate greatly throughout the day.11,12 Zonulin antibodies in the blood may be more stable and reflective of intestinal permeability, but these obviously will not be included on a stool test.
Does the stool microbiome actually reflect the gut microbiome?
You might recall a study that I reviewed and discussed on Chris Kresser’s podcast, which suggests that stool samples don’t accurately reflect the gut microbiome, and tend to over or underrepresent different genera from even the most distal part of the colon.
But this doesn’t mean that stool testing is useless. Consider that the majority of published research on the human gut microbiome to date is on fecal samples. In fact, given the current lack of human studies on the gut mucosa, a stool sample is likely more clinically useful than a small intestinal microbial biopsy.
If you think about it:
- We know how certain interventions like diet, exercise, and antibiotics affect the fecal microbiome.
- We know which fecal microbiome patterns are correlated with certain diseases
- We have a general idea of which microbes should make up the bulk of a healthy fecal sample
- We have a general idea of which microbes should not be present in large amounts in fecal samples.
This means that while fecal samples are imperfect, they are still a useful proxy for the overall ecosystem and are currently one of the best ways to screen for various gut pathologies.
Summary: tests I currently recommend and use myself and with clients
In summary, comprehensive stool tests and microbiome tests can be very helpful tools, but it’s essential to know which ones are reliable, and how to use the information appropriately. The testing landscape is constantly changing, so I am always re-evaluating different stool testing options and will attempt to keep this article up to date with what is available!
I have no affiliation with any stool testing companies. As of this writing, I recommend:
1) Genova GI Effects Comprehensive Profile
This test provides the most comprehensive look at the overall gut environment, parasites, and gives a decent look at bacterial balance. If you’re new to exploring gut health and are only going to get one test, I’d go with this one.
GI Effects is available through many functional medicine practitioners, or direct-to-consumer via directlabs.com (Click on “Order Tests” and search for “GI Effects”).
I recommend the 3-day stool collection if this is your first comprehensive stool test, as it is slightly more thorough in looking for parasites. Results typically take 2 weeks.
2) Thorne Gut Health Test + Genova GI Effects Comprehensive (or CSAP)
For a deeper dive into gut health, I recommend combining the Thorne Gut Health Test with the GI Effects, or another test that will provide clinical information about the gut environment, like the CSAP (just be sure to ignore the culture section!).
Thorne provides the best and most thorough look at the gut microbiome, with extensive raw data that includes overall bacterial balance and the ability to screen for stealth infections. The Thorne Gut Health test is available directly from their website for $198. Results typically take 4-8 weeks.
Unfortunately, the consumer report from Thorne is pretty limited. If you’d like help exploring and understanding your raw data, this is something that I do as part of my 1-on-1 health consultations.
Have you had comprehensive stool testing? Please share your thoughts or experience in the comments below!

About Lucy
Lucy Mailing, PhD is an independent microbiome researcher and gut health science educator. She writes evidence-based articles about the microbiome, gut health, and nutrition science, inspired by her own health journey overcoming chronic eczema.





Thoughts on Tiny Health Pro Gut test?
Great summary. I like knowing about the direct to lab purchase options. Would love to see an update if one is in the works
What is your opinion on fecal secretory IgA testing?
How can I speak to you,Lucy !! I have sibo mathan dominant, very sick a long time,id like to know some information,I see it site very much important, thanks
I’d like to get a virtual 1:1 after ordering the kits you mentioned. My primary focus is seeing how bad my sucralose consumption has affected my gut. I am hoping water kefir and fermented foods allow me to get away with sucralose, as it’s in a lot of my favorite protein brands. Is this something you can help me figure out if I get the test results from the two tests you mentioned?
It’s been a few years since this report was updated and I know this tech has been advancing quickly. The metatranscriptomics technology was new before but I’m hoping we can utilize it better now to provide more detailed insights into gene expression which can be more informative for ongoing health monitoring. Viome claims this is a truly personalized approach so I’m wondering if you have changed your opinion on their testing regime?
What are your thoughts on the Injoy guy microbiome test? They use three samples and ask you to log foods and any symptoms like bloating, gas etc. via an app. This company is fairly new and I believe the test was launched in 2023.
Are you familiar with the company Navipoint for gut health testing?
Hi Lucy! Thank you for this very clear and concise comparison. Are you planning an update here, or is there an updated version on your Patreon?
@Halil – I’m perplexed as to why Thorne would intentionally choose not to provide a sample report of their test on their website. I did find an overview of the test here, with a section for 11 common pathogenic bacteria and parasites seen at 18m26s – https://youtu.be/YWMc5qPv84I?si=RQYXabv7mDSQoBqN&t=1106.
The Thorne test is quite comprehensive and there are additional viruses and fungal species assessed for in it, but it appears that you need to go into the raw data Excel file to have a look at those. That said, I would certainly hope that anything that shows up at a high level would be included the summary report…
Hi Adam
Did you order the test. If so what are your thoughts about it?
The Thorne website does not provide a sample report of their test. Is there a sample report out there that I can have access to? I’m looking to test someone as a donor for FMT and can’t use local labs. I was leaning towards GI Map because this test is exactly ideal for FMT for what they’re testing for but it seems it’s not a reliable test and there’s even a study that says it has a 26% false positive. Does the Thorn test pathogenic bacteria and viruses. The main ones I can think of are; C. Diff toxins A+B, Enteropathogenic E. Coli, Salmonella, Shigella … Parasites (Giardia, Cryptosporidium). Viruses (Adenovirus and Rotavirus). Covid (SARS-CoV-2).
Thank you
How do you rate the biomesight stool test? What are the advantages and disadvantages please?
Very interesting. Thank you for sharing your research! In regards to your comments on the culture – I’m looking at your top choice the “Genova GI Effects Comprehensive Profile” and I notice Candida is in that section. Do you feel the Candida culture is reliable (as opposed to the bacteria culture which you commented on) or is that also unreliable and would warrant using the KOH add on instead? Thanks again!
I recently just did the Diagnostechs GI test, and it seems like they only use the stool culture for the microbiome part and in that section it said I have heavy growth of E. Coli, Citrobacter Braakii, and Staph Aureus.
Should I just completely ignore that entirely? Seems like the rest of the test is accurate but I’m quite unsure as my ND ordered it for me, but I don’t see reviews of it anywhere. I trusted her, she said it was better than the GI map test but I don’t know about that. Maybe it’s a good test, and now I should just do the Thorne microbiome test to complete it?
If you have any information to help please let me know. I hope I didn’t just fundraise $325 for a stool test that was a complete waste….
I completed a Genova GI Effects 3-day comprehensive test at the beginning of the calendar year. Unfortunately, I did not get much information at all from the functional doctor who ordered my test. I think this holds some answers to solving some of my gut issues. I’d like to work with you or someone that can confidently give me solid advice and a direction to pursue. Can you provide any feedback on when you will have more openings on your calendar and perhaps return to your normal hourly rate? If this isn’t in the near future, I would also appreciate any suggestions on someone else who can provide solid interpretations of these test results. Many thanks!
Any review of the TinyHealth microbiome test for babies?
[…] An important first question that should be asked before choosing a microbiome test is what information the tests provide depending on the methods used as microbiome researcher Lucy Mailing explains in her science blog. […]
[…] An important first question that should be asked before choosing a microbiome test is what information the tests provide depending on the methods used as microbiome researcher Lucy Mailing explains in her science blog. […]
[…] Важен първи въпрос, който трябва да си зададете, преди да изберете тест за микробиома, е каква информация предоставят тестовете в зависимост от методите, използвани като изследовател на микробиоми Луси Мейлинг обяснява в своя научен блог. […]
[…] An important first question that should be asked before choosing a microbiome test is what information the tests provide depending on the methods used as microbiome researcher Lucy Mailing explains in her science blog. […]
[…] Una primera pregunta importante que se debe hacer antes de elegir una prueba de microbioma es qué información proporcionan las pruebas dependiendo de los métodos utilizados como investigadora de microbioma Lucy Mailing explica en su blog de ciencia. […]
Great overview, thank you! But there is a discrepancy with what is stated about PCR in your guide and what is stated elsewhere about the CSAP: https://www.doctorsdata.com/Comprehensive-Stool-Analysis-Parasitology-CSAP21: Here it says that this uses PCR ALSO. (And there is a typo: “Clinical markers: No”, but in the title you say that it is a good choice for clinical markers. Best, Inge
Is there a company in the U.K. that does the equivalent of the Genova test? Thank you for your help.
I would like to go with the Thorne test but it says 18 years and up. My kid is 17 and 4 months. If it is weight based he is 95lbs. Is there any concern about using it for younger people?
I really appreciate this information and would like to choose a stool test ASAP. I am stuck between the two top choices. Is there a way to figure out which is right for me? Do they answer different questions? I would love a side-by-side comparison or just a rule of thumb. Thank you!
Hi Deborah! If you are looking for clinically actionable information and have not previously had any comprehensive stool testing, I would generally start with the Genova GI Effects. The Thorne test is best for a more detailed look at the microbiome.
is there any companies that do metagenomics tests in the uk?
Hi Peter. There is a new test, myBiome by SYNLAB (https://www.mybiome.health/), which is offering metagenomics in Europe. I believe you can get it from the UK as well. I don’t yet know whether they will allow access to the raw data, but their reports are quite comprehensive! When I know more, I will update the article to include this option.
ICYMI: the Microba platform from Australia is available in the US now through an outfit called Psomagen. Though it may not belong in your “popular” bucket (it’s fairly new).
Certainly interested in yours’ and others’ opinions, but so far my takes are:
* It’s offering metagenomics with reporting similar to Aperiomics at much lower cost (they seem to have caught the wave of the falling prices you note)
* It offers some pathway analysis atop the metagenomics, which seems pretty robust (not wildly fluctuating) in my repeated tests; but I don’t have a benchmark
* As you noted, a limitation of this approach is that it misses smaller taxa which may be significant
* Similar to Thorne and others, the nutritional recommendations may not be very personalized nor evidence-based
Over multiple tests the reports showed my biome had growing histamine production and it steered me to a specific probiotic to target atop. The probiotic was detected when I was on it and indeed this did turn out to be pretty clearly helpful for a number of my health issues/symptoms. So I will give it credit for that!
What about testing for brachyspira? https://gut.bmj.com/content/70/6/1117
Hi Mark, great question! Brachyspira can be detected in the Thorne raw data. Here is an excerpt from a Patreon post I wrote about that particular study last year that may also interest you:
“While this study is certainly intriguing, I’m not quite ready to say that Brachyspira is a cause of IBS, or even requires direct treatment. Much like Blastocystis, it seems plausible that reduced gut immune function or altered gut mucus dynamics in IBS may simply allow these microbes the opportunity to colonize. Many non-industrialized or rural populations have been shown to have detectable Brachyspira in fecal samples, and a quick look through the metagenomic data I’ve collected from clients over the years shows that many individuals do have detectable Brachyspira – both those with IBS symptoms and those with no gut symptoms! Until we understand more, supporting optimal gut immune function may be the best course of action for those with Brachsypira.”
(Full post can be found here: https://www.patreon.com/posts/gut-research-in-44704838 )
What are your thoughts on fecal mi-RNA testing?
I’m not aware of available clinical fecal miRNA tests yet, but I’ve been feeling jaded about stool microbiota testing of all sorts after reading several fecal/blood miRNA studies done in animals. It seems they show miRNA evaluates the behavior of the microbes, which may provide more practical insight than just their presence (except, I assume, in some cases like parasites).
Hi Elyse – yes, fecal mi-RNA testing is only being done in the research setting at the moment, and is not available clinically. It may someday provide more information about microbial behavior! For the time being though, the presence of microbes and their relative abundance is still practically useful, especially in screening for major pathologies.
I am considering Aperiomics.To use analogy, their sample would tag every pathogen they find, but not the benificial pathogens. To me, this would seem to be like an aerial photograph with a star on each undesirable plant or tree, but no markings on the desirable ones. So you would know what the camera could see, but not how it is interlaced with the entire ecosystem and thus the severity of effect of the pathogen on the system and its makeup. A patch of Kudzu is a bad thing, but is a little English Ivy a signal to act? And the true nature of the system may not be evident by identification alone, the interaction being invisible to the camera (the test results). A totally accurate and detailed report of a battlefield, for example, can only indicate how the skirmish might progress by seeing what is where and where it is likely to go from there. Um………
What are your thoughts that Dr. Mark Pimentel does not find GI MAP reliable and neither does microbiologist Kiran Krishnan?
Hi Bete,
Thanks for your comment! I am no longer using GI-MAP and haven’t for over a year since I discovered issues with test reproducibility. I’ll be posting an update to this article in the near future!
Hi Lucy,
Thank you for you amazing research! You are my goto for suggestions based on research. ;-)
Do you have an update to your favorite stool testing? I know science and research is always improving. As a practitioner, I am always learning and would love to hear your latest suggestions.
Thanks for your comment, Ali! It has been updated :)
Hi Lucy, You mentioned you’re no longer using GI Map. What is your best recommendation for testing now, particularly for those with suspected IBS/SIBO? I couldn’t find an update to this article.
Thanks for your comment, Toffler! It’s been updated now :D
Any comments on Viome test in comparison to others?
Hi Teresa. Viome is using meta-transcriptomics, which cannot currently provide any clinically useful information. They also cannot determine bacterial abundances from the transcriptome alone.
Very well-researched information!
Can you give any examples of gut pathogens that Aperiomics has caught that other technologies could not?
As always, a well-researched and comprehensive report.
Having now done six Biome tests and one Thryve, I am not really sure that 16S rRNA sequencing is that reliable. For example, I sent two almost identical samples sent to Thryve and Ubiome to see what results I got.
Of the organisms that both found, the proportions differ dramatically. Just looking at the phylum level, we get these results:
Ubiome Thryve
Actinobacteria-phylum 2.781% 1.149%
Bacteroidetes-phylum 42.563% 46.499%
Firmicutes-phylum 45.617% 39.940%
Proteobacteria-phylum 4.296% 7.552%
Verrucomicrobia-phylum 4.744% 4.739%
These are significant proportions of the microbiome. Yet the only one that is reasonably close is Verrucomicrobia (mainly Akkermansia). The major phyla Bacteroidetes and Firmicutes vary by 9% and 14% respectively. Proteobacteria, an important phylum because of the negative effects of its members, varies by 76%, which in comparison terms means Thryve found almost twice as many organisms as Ubiome. Similarly, Ubiome found almost 2.5 times as many Actinobacteria.
When you start to look at the lower levels, you see even greater discrepancies. Ubiome found 395 times as much Pseudobutyrivibrio as Thryve. (2.141% vs 0.005%)
In fact, only 18 of the 166 taxa both detected were within 10% of each other. Only 44 were between 10% and 100% of the other. A worrying 49, almost a third, were greater than 1000% different!
Than consider the organisms found by one but not the other. Thryve found Sporobacter termitidis to comprise 1.4% of the total microbiome. Ubiome found none. But Ubiome found Streptococcus sp. 2011_Oral_MS_A3 to comprise 4.6% of the total microbiome while Thryve found none. It is mind-boggling that such large percentages can be completely missed.
There are many reasons why this might be the case, apart from possible variation in the stool itself.
1. Thryve finds many more taxa than Ubiome (673 vs 234). Thryve compares their results against many more databases than Ubiome, so likely will find more named organisms. However, Ubiome also reports organisms that Thryve does not, so Ubiome’s databases are not a subset of those used by Thryve. One has to wonder why these companies are not using a single comprehensive database to produce more useful and comparable results.
2. The machines use a number of probes that are sensitive to different organisms. If Thryve uses more probes, or different probes, they will find more and different types of organisms than Ubiome. But Ubiome must use different probes because Ubiome finds some organisms that Thryve doesn’t.
3. The two companies seem to have different ideas of what makes a significant result. Thryve reports organisms for which it has counted at least one. Ubiome only reports those for which it has found two or more. One has to ask whether relying on a single example of an organism is meaningful – could it just be a reading error? 226 of the 673 Thryve taxa rely on a single organism being detected.
And comparing the taxa found in my various samples, I find taxa appearing and disappearing regularly. My latest Ubiome found 18 taxa that I had never seen in earlier Ubiome tests or in Thryve. My feeling is that this method of testing is pretty hit-or-miss. Even if you can get a good sample from the stool, what is reported is likely only a proportion of what is actually in your stool.
If you use the same company for a sequence of tests, you have a better chance of comparable results. But do not consider that you have anywhere near a comprehensive picture of your stool microbiome. Perhaps the phyla might be something you can work with, but anything below that would need careful consideration.
Great info David, thanks.